Quality indicators in esophagogastroduodenoscopy
Article information
Abstract
Esophagogastroduodenoscopy (EGD) has been used to diagnose a wide variety of upper gastrointestinal diseases. In particular, EGD is used to screen high-risk subjects of gastric cancer. Quality control of EGD is important because the diagnostic rate is examiner-dependent. However, there is still no representative quality indicator that can be uniformly applied in EGD. There has been growing awareness of the importance of quality control in improving EGD performance. Therefore, we aimed to review the available and emerging quality indicators for diagnostic EGD.
INTRODUCTION
Esophagogastroduodenoscopy (EGD) is an important procedure for the diagnosis of upper gastrointestinal (GI) diseases. EGD is also used as a screening modality for the diagnosis of upper GI cancers in high-risk areas.1 The main purpose of EGD in a screening setting is to enhance the detection rate of early stage gastric cancers and to reduce cancer-related mortality. Several recent studies have reported various quality indicators for EGD.2-8
Quality standards can be subdivided into domains of structure, procedure, outcome, and adverse events.3,5,6,8 The structural domain reflects whether the facilities and equipment at the endoscopy unit are satisfied. The procedure domain refers to whether certain procedures before, during, and after EGD are being carried out to avoid missed diagnosis and increase patient tolerance. Performance variability among endoscopists can affect the outcomes. The outcome domain is generally considered the most important, and it reflects the effectiveness of EGD, such as the detection rate of premalignant lesions or cancer.
An ideal quality indicator for EGD should be highly associated with cancer incidence and mortality after endoscopic examination. Adenoma detection rate is a representative quality indicator of colonoscopy.9 Measurement of cecal intubation rates, mean withdrawal time, and bowel preparation quality are also important quality indicators of colonoscopy.10-12 These indicators strongly correlate with the risk of interval colorectal cancer and patient mortality. In contrast to colonoscopy, there are no representative quality indicators for EGD. The complex secretory function and peristaltic folds of gastric mucosa make its observation a challenging procedure. Precancerous neoplasms often exhibit subtle morphological changes during EGD. In particular, gastric neoplasms are commonly accompanied by severely inflamed background mucosa, caused by Helicobacter pylori gastritis, making it more difficult to detect the gastric lesions.13,14 Several studies have reported that the average rates of missed upper GI cancers during EGD are greater than 20% in Asia and 7.2%–14.0% in the West.15-18 Therefore, accurate diagnosis relies on careful mucosal scanning.
Therefore, we focused on the domain of endoscopic procedures and outcomes, among various quality indicators, which are directly related to the endoscopic detection of early gastric cancers at an individual endoscopist’s level.
PREMEDICATION
Poor preparation prior to EGD may interfere with concentrated visualization. Premedication for endoscopic examinations consists largely of mucolytic, defoaming, antispasmodic, and sedative agents. Previous questionnaires have reported discrepancies in the frequency of premedication use worldwide.19
Mucolytic and defoaming agents
Proper bowel preparation increases the diagnostic yield of colonoscopy.20 The importance of adequate mucosal preparation using mucolytic and defoaming agents has yet to be proven, although cleansing of mucus, bubbles, and foam is important for clear mucosal observation during EGD. Pronase, or N-acetylcysteine, is a mucolytic agent used to eliminate gastric mucus. Simethicone (activated dimethicone) is a commonly used defoaming agent that decreases the surface tension of gas bubbles without significant adverse interactions.21 Therefore, combining mucolytic and defoaming agents has been shown to be effective in improving the visibility of the gastric mucosa when used 20 min prior to EGD.22-24 A recent study showed that pronase significantly enhanced the visibility of all anatomical sites of the upper GI tract when compared with a control using water (p<0.001).23 However, this study did not demonstrate whether premedication with pronase and simethicone increases the detection rates of gastric neoplasms or precancerous lesions by experienced endoscopists. Considering the potential risk of missing lesions by inexperienced endoscopists,25 adequate mucosal cleansing can improve visualization of the gastric mucosa and result in superior diagnostic yield. However, the optimal quantity, density, and administration time of premedication have not yet been established.
Antispasmodic agent
Endoscopic stimuli during EGD further increases peristalsis, making it difficult for endoscopists to obtain static images and observe the detailed mucosal surface without blind areas. Therefore, antispasmodic agents, such as cimetropium bromide, scopolamine, and hyoscine N-butylbromide have been commonly used to reduce peristalsis during EGD in clinical practice. A recent Asian consensus recommended the use of antispasmodic agents (especially topical peppermint oil) during EGD to enhance the detection of precancerous neoplasia. This was based on a paucity of evidence.7 The consensus commented that gastric cancer in the greater curvature, even an advanced one, could be missed if the gastric wall was not fully distended. A recent propensity score-matched study in Korea showed that cimetropium bromide use was significantly associated with increased gastric neoplasm detection rates, especially for lesions in the stomach body (gastric neoplasm detection rate, 0.30% [cimetropium bromide users] vs. 0.19% [non-users]; p=0.02).26 A Japanese study reported that premedication with scopolamine did not significantly increase the detection rate of upper GI neoplasia (upper GI neoplasia detection rate, 0.42% [scopolamine users] vs. 0.39% [non-users], p=0.89).27 There is no objective classification for the measurement of peristalsis, and different individuals might have different responses to antispasmodic agents. Therefore, future studies are required to evaluate the association between the degree of antiperistaltic activity of antispasmodic agents and the detection rate of upper GI neoplasia. Contraindications to the use of antispasmodic agents should be carefully considered because their routine use can raise safety concerns, such as arrhythmia, benign prostate hypertrophy, and glaucoma.
Sedation
Sedation is widely used during upper GI endoscopy. Sedation is used in more than half of EGDs in European and Asian countries, and more than 90% in the United States (US).19,28 Sedation reduces patients’ anxiety, which possibly allows endoscopists to thoroughly observe the stomach with sufficient time,29-31 thereby improving the quality of EGD. A meta-analysis showed that when compared with non-sedation, moderate sedation during EGD significantly improved patient satisfaction (relative risk [RR], 2.29; range, 1.16–4.53) and willingness to repeat EGD in the future (RR, 1.25; range, 1.13–1.38).29 However, the role of sedation on the endoscopic detection rate is currently unclear. This lack of evidence leads to questions regarding the direct relationship between sedation and the endoscopic findings. A recent propensity score-matched cohort study showed that propofol-based sedation separately and significantly enhanced the detection rate of early esophageal cancer (p=0.044), early gastric cancer (p=0.020), esophageal high-grade intraepithelial neoplasia (p<0.001), and gastric high-grade intraepithelial neoplasia (p=0.042), when compared with non-sedation during EGD.32 In the sedation group, gastric high-grade intraepithelial neoplasia and early cancer were detected more frequently at the gastric body (p=0.001). This may have resulted from the increasing application of supplementary endoscopic techniques, longer observation times, and more biopsies at different sites. No significant difference was observed in the overall number of precancerous lesions and low-grade intraepithelial neoplasia. Further prospective randomized case-control studies are needed to assess the use of sedation as it improves patient tolerance and the detection rate of upper GI neoplasia.
PHOTODOCUMENTATION
Photodocumentation has become an important aspect of EGD reporting. Although appropriate photodocumentation seems to be related to EGD diagnostic efficiency, no data support a direct relationship with EGD quality improvement. During EGD, certain locations, such as the posterior wall, cardia, and greater curvature of the body are difficult to visualize.17
The minimum requirements for photodocumentation vary worldwide and reflect the different incidences of upper GI cancer in different areas. In the US, the guidelines do not specifically indicate the minimum number of images for EGD reports.3 Conversely, the European Society of Gastrointestinal Endoscopy (ESGE) proposed that photodocumentation in a normal endoscopic examination should have at least 10 images, including anatomical landmarks to illustrate the examination, namely: (1) upper esophagus; (2) lower esophagus; (3) squamocolumnar junction and diaphragm indentation; (4) cardia and fundus in inversion; (5) gastric body in forward view, including the lesser curvature; (6) gastric body in retroflex view, including the greater curvature; (7) angulus in partial inversion; (8) gastric antrum; (9) duodenal bulb; (10) second part of duodenum (Fig. 1).8 Korean and Japanese doctors usually take 20–40 endoscopic images during EGD screening. The Korean Society of Gastrointestinal Endoscopy (KSGE) recommends photodocumentation of at least eight images in a normal EGD examination, with additional images of suspicious lesions.6 In Japan, a “systematic screening protocol for the stomach (SSS)” that includes 22 images was suggested to study the entire stomach.33 This protocol was developed to avoid blind spots by presenting a required minimum standard; however, it is rarely used in the West. A recent study reported a positive association between the number of endoscopic images and the detection rate of clinically significant gastric lesions (p<0.001).34 However, endoscopists who took more images tended to have longer observation times and performed more biopsies than endoscopists who took fewer images in this study. Therefore, the level of interest and effort of endoscopists may be related to the acquisition of more images and the detection of more lesions. Moreover, it is possible that the number of endoscopic images and observation time increased because of suspected lesions. Knowing that the number of images taken during endoscopy is monitored, endoscopists may take more irrelevant images without a positive effect on the outcome. Currently, no well-designed studies have examined the relationship between the number of images and the detection rate of neoplasia during EGD.
Photodocumentation of anatomical landmarks is considered to be a proof of complete examination. A Korean study proposed the visualization of the major papilla in the duodenum as a quality indicator, as it reflects an endoscopist’s skillfulness and attention during examination.35 This study showed a positive correlation between high ampulla observation and detection rate of total upper GI neoplasia, and recommended a minimal threshold of 50% for ampulla image documentation rate (R2=0.57, p=0.03). Therefore, photodocumentation of the duodenal ampulla can serve as an auditable measure of performance for completeness of EGD. As another landmark image, the British Society of Gastroenterology (BSG) recommends photodocumentation of an inlet patch.5 An inlet patch can easily be missed with rapid withdrawal of the endoscope because it is located just below the upper esophageal sphincter. Therefore, the identification of an inlet patch can be used as a surrogate marker for a complete procedure of the esophagus, although the level of recommendation is weak in this guideline. Therefore, systemic mapping to avoid blind areas and photodocumentation of surrogate markers, such as the duodenal ampulla or inlet patch could be considered as quality indicators in EGD.
REPORTING
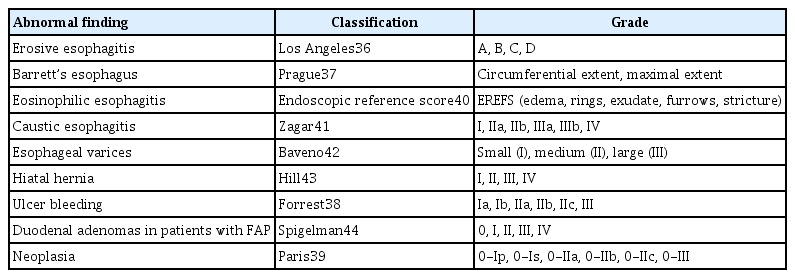
Accurate endoscopy reports are key performance measures for EGD.5,6,8 The ESGE recommends the correct use of validated terminology for specific diseases, which is considered to be a hallmark for quality improvement.8 Moreover, the use of classification systems in endoscopy enables better communication between endoscopists for abnormal endoscopic findings, treatment, and clinical recommendations. There are well-established endoscopic classifications, such as the Los Angeles classification for erosive reflux disease, Prague classification for Barrett’s esophagus, Forrest classification for ulcer bleeding, and Paris classification for early neoplastic lesions.36-39 The standardized classification systems are presented in Table 1.36-44 The implementation of these classifications may not be straightforward because of inter-observer variability. The BSG also suggested that accurate reports of major EGD findings and key recommendations should be produced contemporaneously.5 The recommended interval or any instructions to the patients should be recorded if follow-up examinations or changes in medication are required. To monitor reporting as a performance measurement, a systematic electronic reporting system should be developed that includes pathology data, adverse events, patient satisfaction, and surveillance intervals.
OBSERVATION TIME
Adequate observation time plays an important role in enhancing the detection rate of upper GI neoplasia.7,8 Observation time is one of the most subjective endoscopist-dependent factors. A multicenter prospective study from the US, which included 112 patients with Barrett's esophagus who underwent surveillance endoscopy by 11 endoscopists, showed that prolonged inspection time (>1 minute per centimeter) in Barrett’s esophagus was associated with an increased detection of high-grade dysplasia or adenocarcinoma (p=0.04).45 Therefore, longer inspection time can be a widely available method to enhance the yield of cancer surveillance in Barrett’s esophagus. However, the clinical significance of longer inspection time during EGD screening in asymptomatic patients remains unclear. A single-center study conducted in Singapore was the first report on the detection rate of gastric lesions with respect to observation time.46 This study investigated detection rate of high-risk gastric lesions, such as atrophic gastritis, intestinal metaplasia, dysplasia, and cancer by 16 endoscopists, including trainees, among 837 symptomatic patients. Slow endoscopists, who took more than 7 minutes to perform an EGD, were twice as likely to detect high-risk gastric lesions than faster endoscopists (odds ratio [OR], 2.50; 95% confidence interval [CI], 1.52–4.12) and three times more likely to detect dysplasia or cancer than faster endoscopists (OR, 3.42; 95% CI, 1.25–10.38). Of the 837 patients in this study, only 11 cancer and eight dysplasia cases were detected. Moreover, the study conducted in Singapore targeted symptomatic patients and included an endoscopy trainee; therefore, generalizability of the study was limited. A retrospective study conducted in Japan revealed a positive relation between the endoscopist observation time and neoplasm detection rate.47 However, confounding variables that have a significant effect on the development of gastric cancer, such as smoking, body mass index, H. pylori infection, and family history of gastric cancer were not adjusted in this study. In a retrospective Korean study, the data of 111,962 patients, who participated in a seven-year long health-screening program, were analyzed.48 In this study, the observation time was calculated from the time of withdrawal of the endoscope from the second part of the duodenum to the end of EGD examination, a concept similar to the observation time used in colonoscopy. Using a cutoff of 3 minutes, eight endoscopists were classified into the fast group (mean examination time, 2:38±0:21 minutes) and six endoscopists were classified into the slow group (mean examination time, 3:25±0:19 minutes). The study showed that the slow endoscopists detected more gastric adenomas or cancers than the fast endoscopists (0.28% vs. 0.20%; p=0.0054). Additionally, most confounding variables related to the development of gastric cancer, such as age, sex, body mass index, diabetes mellitus, family history of gastric cancer, presence of symptoms, and presence of H. pylori infection, were reflected. It was necessary to verify whether the detection rate improved with an increase in observation time. Therefore, the same researchers further investigated whether implementing an institutional policy of spending at least 3 minutes for EGD observation would improve the detection rate of upper GI neoplasia.49 This study demonstrated that the institutional protocol could increase the detection rate of upper GI neoplasia by 38%, especially in gastric dysplasia. However, the detection rate of upper GI neoplasia did not increase proportionally with longer observation time (>3 minutes). The implementation of institutional policy, requiring all endoscopists to spend more time for observing the upper GI mucosa, improved upper GI neoplasia detection rate; however, this was not statistically significant at each endoscopist’s level. These results may be due to the relatively small number of upper GI neoplasias detected during diagnostic EGD compared to colonoscopy, or due to the ceiling effect of EGD observation time. Therefore, further studies should be conducted using several cutoff observation times. An overview of studies on the association between observation time and neoplasm detection rate in EGD is presented in Table 2.45-49 A single-center retrospective study investigated the detection rate of synchronous gastric neoplasm according to observation time in patients who underwent endoscopic resections.50 In accordance with earlier studies on health-screening endoscopy,45,47,48 within one year of follow-up examination after endoscopic resection, multiple synchronous gastric neoplasms were found more frequently in examinations observed for a longer time. In other words, a longer observation time is required, particularly for high-risk patients. Overall, the observation time was an independent factor that determined the quality of EGD.
BIOPSY RATE/PROTOCOL
Endoscopic biopsy plays a major role in the diagnosis and surveillance of precancerous lesions, with high sensitivity and specificity. For the histopathological diagnosis of a suspected malignant lesion, at least four to eight multiple biopsies are usually recommended. However, multiple biopsies may increase the procedure time, bleeding risk, medical costs, and workload of pathologists. Usually, three or four biopsies of a lesion are considered as the optimal number for accurate diagnosis. A Korean study revealed that additional biopsies taken from the same site did not improve the diagnostic accuracy.51 A more important factor is the exact targeting of appropriate site and acquisition of viable tissue. In a previous study, specimens obtained from the inner margin of the ulcer showed a more accurate diagnosis than those from the ulcer base.52 An EGD with a carefully targeted biopsy can improve the diagnostic process; therefore, it should be performed to improve the quality of endoscopy. Additionally, an image enhanced endoscopy (IEE)-assisted biopsy could make it easier to perform a targeted biopsy and decrease the number of biopsies for histopathological diagnosis.7,53
A Korean study found that the endoscopic biopsy performance rate varied widely among endoscopists (range, 6.9%–27.8%) and was significantly associated with the detection rate of upper GI neoplasia (R2=0.76; p=0.0015).48 Conversely, a multicenter European study that analyzed outpatient EGD data showed that endoscopists with a high endoscopic biopsy performance rate had a lower rate of missing the gastric cancer diagnosis than those with a lower endoscopic biopsy performance rate.54 This is because the increase in endoscopic biopsy rate could result in an increased rate of negative biopsy. This study suggested that a biopsy rate between 43.8%–51.6% could maintain the optimal balance between efficacy and cost. However, using the absolute value of biopsy rate as a quality indicator needs to be studied further, because the prevalence of precancerous lesions or gastric cancer is dependent on the region or country. Therefore, the endoscopic biopsies that are performed in the same endoscopy unit/region should be assessed to identify endoscopists requiring improvement and to maintain high diagnostic performance.
The prevalence rates of Barrett’s esophagus have progressively increased in the West, but remain low in Asia.55,56 Most cases in Asia are of short-segment Barrett’s esophagus that is associated with a limited risk of esophageal adenocarcinoma.55 Therefore, interest in Barrett’s esophagus and the endoscopic or histopathological diagnostic criteria for this differ from region to region. For surveillance of Barrett’s esophagus, the Seattle protocol suggested obtaining four quadrant biopsy samples every 1–2 cm along the columnar-lined esophageal segment.57 The ESGE, American Society for Gastrointestinal Endoscopy (ASGE), and BSG recommended the use of Seattle biopsy protocol for diagnosing Barrett’s esophagus. However, the Asian consensus and KSGE have not provided any guideline for the biopsy protocol for Barrett’s esophagus. Surveillance of Barrett’s esophagus is still controversial because of its low prevalence and the lack of randomized trial studies in Asia.
The updated Sydney system is the most widely accepted protocol for gastritis classification and grading. This system recommends taking at least five biopsies: two from the antrum (from the greater and lesser curvature, 3 cm from the pylorus), one from the incisura, and two from the body (from the lesser curvature, 4 cm proximal to the incisura, and from the greater curvature, middle).58 Moreover, in patients with advanced stages of gastritis, other histopathological staging (Operative Link on Gastritis Assessment [OLGA] and Operative Link on Gastric Intestinal Metaplasia [OLGIM] assessment) can be used to stratify the risk of cancer progression.59 The European consensus on “Management of precancerous conditions and lesions in the stomach” (MAPS II guideline) suggested a three-year interval strategy for endoscopic surveillance of advanced stages of atrophic gastritis (severe atrophic changes or intestinal metaplasia in the stomach’s antrum and body, OLGA/OLGIM III/IV).53 However, some areas in Asia, especially in Korea, most of the population has easy accessibility to endoscopic surveillance, as the national cancer screening program is conducted more frequently than every three-year interval. Therefore, in this specific area, the intervals or methods of endoscopic surveillance can be adjusted rather than completely following international guidelines.
ENDOSCOPY EDUCATION
Intensive training or education can play an important role in improving the quality of EGD. Improvements in the detection rate are not solely determined by the number of EGDs performed. It requires a strong awareness of benign and malignant lesions, a good ability to identify early cancer, and an effort to standardize endoscopic examination. A retrospective study in China investigated whether specific training enhanced the detection rate of early gastric cancer.25 During three consecutive training periods of eight months (period 1), four months (period 2), and four months (period 3), skilled endoscopists (who performed >3,000 EGDs) participated in voluntary training programs, which included discussion of cases or published articles, education on standard endoscopic examination, and communication between endoscopists and pathologists. The detection rates of early gastric cancer during first, second, and third periods were 0.3%, 0.6%, and 1.5%, respectively. Intensive training in these aspects dramatically improved the quality of endoscopy even for skilled endoscopists. A Japanese study also showed that two years of intensive training for accurate diagnosis of early gastric cancer dramatically improved its detection rate when compared with that before intensive training (0.4% vs. 1.9%, p<0.01).60 Continuous endoscopy education should focus on improving technical skills and knowledge. To date, no qualified on-site training center exist in Korea. Instead, KSGE has provided a web-based learning program for the quality control of endoscopy.61 Since 2013, the Korea National Cancer Center has also been offering education to improve the quality of endoscopic cancer screening.62 On-site teaching could achieve higher educational goals than web learning, but the latter is advantageous in that it can be easily accessed anywhere and repeated as many times as needed.
IMAGE ENHANCED ENDOSCOPY
The diagnosis of early upper GI neoplasia requires a two-step process: detecting suspicious lesions and differentiating their histopathology. Once a suspicious lesion is identified, IEE techniques can be used for further clarification. IEE plays an integral role in early detection and characterization of neoplasia, based on its surface structure and microvasculature. There are two major types of IEE: chromoendoscopy and equipment-based IEE.63 Of these, equipment-based IEE has recently been developed and has various features, such as magnifying endoscopy with narrow-band imaging (ME-NBI), flexible spectral imaging color enhancement, blue laser/light imaging, and i-SCAN, depending on the endoscope manufacturer. Along with technological progress, knowledge of the modalities and clinical practicality of IEE is presumed to be essential in clinical practice. To date, this novel equipment has mainly been used in general to tertiary medical centers. Although it is not available in primary clinics, it seems to have enormous potential for widespread use. Correct diagnosis rate of early gastric cancer can be increased after educational lectures on the classification system of microvascular and microsurface patterns, using ME-NBI, regardless of board-certification status.64 Additional education for novel image enhancement techniques may improve the accuracy of endoscopy-based diagnosis, even in skilled endoscopists.
ARTIFICIAL INTELLIGENCE
In the field of upper GI endoscopy, many studies have applied artificial intelligence (AI) in the detection and classification of malignant lesions as well as quality improvement by monitoring the blind areas.65-70 Deep learning is an advanced subclass of AI that logically mimics the activity of neurons on computer algorithms through a convolutional neural network (CNN) system. Among the various types of neural networks, CNN is known to be the best-performing system for computer vision. This discriminative model automatically recognizes anatomical locations, detects lesions, distinguishes boundaries, and predicts classification using archived endoscopic images.66,67,71
The rate of missed gastric cancer cases by EGD is 4.6%–25.8%,15,17,72,73 and one of the main reasons for this is incomplete inspection. A randomized controlled trial from China constructed a real-time quality improving system, named “WISENSE,” based on the deep learning achievements.70 Compared to sedated EGD without WISENSE, sedated EGD with WISENSE assistance significantly reduced the rate of blind spots (5.9% vs. 22.5%), prolonged the mean inspection time (5.03 minutes vs. 4.24 minutes), and enhanced the completeness of image documentation (90.6% vs. 79.1%). In particular, the assistance of WISENSE reduced the incompleteness of observations in the lesser curvature of the fundus and antrum to less than 20% and 4%, respectively. The same researcher also developed a novel AI system named “ENDOANGEL” to further evaluate and compare the performance of sedated EGD, unsedated EGD, and unsedated ultrathin transoral endoscopy (U-TOE) with or without the assistance of this AI system.74 These three types of EGD have different technical aspects that affect the quality of the procedure. With the assistance of ENDOANGEL, the rate of blind spots in sedated EGD was significantly lower than those in unsedated EGD and U-TOE (3.42% vs. 31.23% vs. 21.77%). This was explained by patient-reported comfort scores, which were significantly higher in the sedated EGD group. The blind area rate in the AI subgroup was significantly lower than that in the control subgroup for all three types of endoscopies (sedated EGD, 3.42% vs. 22.46%; unsedated EGD, 31.23% vs. 42.46%; and U-TOE, 21.77% vs. 29.92%). This study suggests that AI-assisted EGD is a practical tool not only in sedated EGD, but also in a less resource-available setting. In another recent study that evaluated the CNN model’s image quality control in EGD, the constructed CNN model classified the EGD images into one of the eight locations of the upper GI tract with 97.58% accuracy and monitored the completeness of the EGD examination with 89.20% accuracy.69 While previous WISENSE and ENDOANGEL were developed based on 22 landmark images of SSS, this constructed CNN model was trained by using the eight landmark images documentation of the ESGE. Recently, the statement paper of the ASGE has provided guidance for clinical application, testing, or validating algorithms for successful implementation of AI in GI endoscopy.75 The advancement of AI applications in endoscopic images would be useful for standardizing practice variations among endoscopists, decreasing workload, assisting in decision-making, and improving the quality of EGD in the near future. The creation of large data sets, successful integration of multicenter data, and control of data noise have still been a challenge to speed up the development of AI for GI endoscopy. In the recognition of these upcoming changes, it might be an optional indicator to assist endoscopists.
CONCLUSIONS
Considering that EGD is a highly endoscopist-dependent examination, optimal quality indicators of EGD could reduce procedural variation among endoscopists and contribute to improving the early detection of upper GI neoplasia. The stage of gastric cancer at diagnosis determines its prognosis.76 Early detection of gastric cancer is an effective method for lowering cancer mortality. It could provide a better chance to treat patients using endoscopic therapy rather than surgery.77 In this review, quality indicators were temporarily classified into premedication, photodocumentation, reporting, observation time, biopsy rate/protocol, endoscopy education, IEE, and AI (Fig. 2). For clear visualization of the area, mucolytic/defoaming or antispasmodic agents should be considered. To enhance the detection rate of upper GI neoplasia, the use of sedative agents, photodocumentation, systemic reporting, and sufficient observation times are recommended. Endoscopy education for accurate diagnosis and a biopsy protocol are necessary to maintain and improve the quality of EGD. Although further validation in actual clinical practice is needed, IEE and AI may have a prominent impact on the improvement of the diagnostic yield.
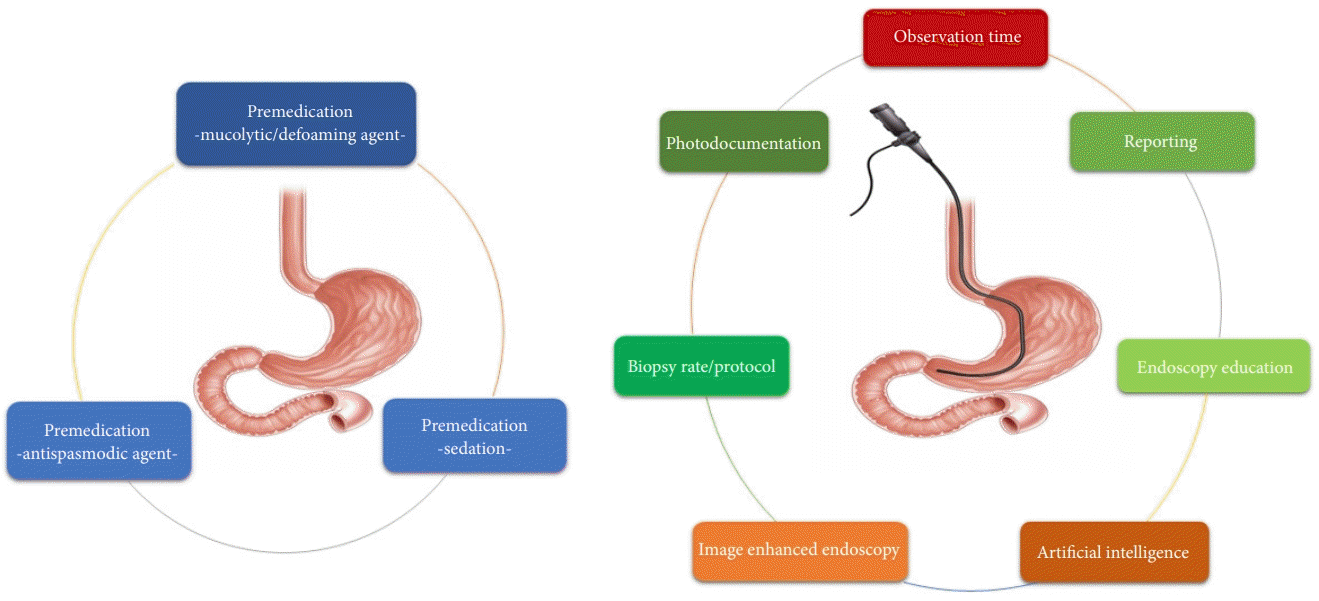
Classification of quality indicators into premedication, photodocumentation, reporting, observation time, biopsy rate/protocol, endoscopy education, image enhanced endoscopy, and artificial intelligence.
Familiarity with these quality indicators is expected to be helpful for endoscopists in performing high-quality EGD examinations; a summary of quality indicators recommended in several published guidelines is presented in Table 3.3,5-8 Some indicators are evidence-based, whereas most are based on expert consensus and may warrant further studies. Refinement of the quality indicators for EGD should consider measurable performance and reflect clinical outcomes.
Notes
Conflicts of Interest
The authors have no potential conflicts of interest.
Funding
This research was supported by the Basic Science Research Program through the National Research Foundation of Korea, funded by the Ministry of Education, Science, and Technology (2019R1A5A2027588 and 2020R1F1A1076448).
Author Contributions
Conceptualization: JMP, SYK; Formal analysis: JMP, SYK; Writing–original draft: JMP, SYK; Writing–review & editing: SYK, JMP. All authors revised the first draft of the manuscript and approved its final draft.