AbstractBackground/AimsPatients may feel embarrassed during colonoscopy. Our study aimed to assess changes in patient preference, over the past decade, for the sex of their colonoscopist.
MethodsProspective studies were performed at a single health center from July to September 2008, and from July to September 2016. Subjects included colonoscopy patients (2008: 354, 2016: 304) who were asked to complete a questionnaire before colonoscopy.
ResultsIn 2016, 69 patients (24.9%) expressed a sex preference, compared with 46 patients (14.6%) in 2008. By 2016, female patient preference for a female colonoscopist had significantly increased to 95% (odds ratio [OR], 2.678; 95% confidence interval [CI], 1.418т 5.057; P=0.002). In multivariate analysis, patient sex (OR, 4.404; P=0.000), patient age (OR, 0.977; 95% CI, 0.961т0.992; P=0.004), and year of procedure (OR, 1.674; 95% CI, 1.028т2.752) were statistically significant factors in sex preference. Between 2008 and 2016, female patients preferred a female colonoscopist because of embarrassment. Male patients also preferred a male colonoscopist, and the primary reason shifted from expertise to patient embarrassment (2008: 29%, 2016: 63%).
INTRODUCTIONColonoscopy is considered the gold standard for colon investigation and is the most effective method for assessing colonic lesions [1]. However, colonoscopy is an invasive and uncomfortable procedure, and patients may feel fear and embarrassment during the examination [2-4]. The number of female gastroenterologists has increased, and the options available to patients for choosing the sex of their healthcare provider are also increasing [5]. In addition, consideration of patient rights and privacy are increasingly important. Therefore, the sex of the colonoscopist has also become increasingly important.
Patient preference for a colonoscopist of the same sex has been demonstrated in Western countries [2,3,6]. Female patients have a stronger preference for a female (53%) versus male (27.8%) colonoscopist, and are willing to wait longer and pay more for their preference [6]. In Korea, only two studies have investigated this issue. In 2005, Kim et al. [7] reported that most male patients preferred a male colonoscopist, whereas half of the female patients preferred a male colonoscopist [7]. In 2008, Lee et al. [8] reported that more than half of the women had no preference regarding the sex of their colonoscopist, and sex preference was related to patient employment status, educational level, age, and marital status [8]. In previous Korean studies, female patients tended to prefer male over female doctors, in contrast to Western countries, because of the social perception that a male colonoscopist is more professional in Korea [7,8]. However, during the last decade, as perceptions on gender equality have improved, the social perception of female physicians has also improved [9]. In addition, according to the Korean Society of Gastrointestinal Endoscopy, the proportion of newly certified female endoscopy specialists has increased in the last 10 years (2006: 19.9%, 2015: 31%). This suggests that the recent demand for female colonoscopists has increased in Korea.
In this study, we assessed patient preference with regard to the sex of their colonoscopist, particularly focusing on changes during the past decade in Korea. Our aim was to evaluate the change in perception concerning the sex of the colonoscopist.
MATERIALS AND METHODSStudy designA single center, prospective study was performed from July to September 2008, and from July to November 2016, at the Department of Gastroenterology and Digestive Endoscopy of Korea University Anam Hospital (Seoul, Korea). In total, 649 patients undergoing colonoscopy were prospectively asked by male and female colonoscopists to complete questionnaires before the procedure. We used the same questionnaire in 2008 and 2016 to investigate changes in sex preference during this 8-year period. All patients provided written, informed consent.
PatientsIn this study, we included all patients aged between 20 and 75 years scheduled to undergo colonoscopy. We excluded patients who were considered to be at risk of undergoing endoscopy for known or suspected gastrointestinal obstruction, ileus, severe heart failure, or uncontrolled hypertension (systolic pressure >170 mm Hg, diastolic pressure >100 mm Hg). This study was conducted in accordance with the Helsinki Declaration and approved by the institutional review board (ED16314) of the Korea University Hospital. We received the preprocedural questionnaire from 345 patients in 2008 and 293 patients in 2016; all were scheduled for elective colonoscopy. Patients undergoing colonoscopy were randomly selected from among 10 patients per day, regardless of indication, underlying disease, history of colonoscopy, outpatient versus inpatient status, sedation, or scheduled colonoscopist.
QuestionnaireAll patients were directly asked by doctors about their preference with regard to the sex of their colonoscopist before the procedure. An equal distribution of questioners of both sexes were used for the study to reduce any variability caused by the questionerтs sex. The questionnaire asked general patient information including age, sex, waist circumference, educational level, history of colonoscopy, and presence of underlying disease. The patients were asked whether they had a preference with regard to the sex of their colonoscopist and the reason for the preference. To evaluate the intensity of the sex preference, patients who stated a sex preference were asked how much time or how many days they are willing to wait for colonoscopy.
Data collectionThe responses were collected and analyzed for raw data associations by a reviewer who was unaware of the patient details. Additional information was obtained from the medical records through the automated Korea University Anam Hospital electronic medical record system.
Statistical analysisContinuous variables were expressed as meanТБstandard deviation, and discontinuous variables were expressed as counts and percentages. SPSS 20.0 for Windows (SPSS Inc., Chicago, IL, USA) was used for data entry and statistical analyses. For the analyses between the two different groups, Studentтs t-test was used to compare continuous variables and the chi-square or Fisherтs exact test was used for categorical data. We conducted a logistic regression analysis to evaluate the correlation between patient sex preference for their colonoscopist and the factors affecting the preference. P-values <0.05 were considered statistically significant.
RESULTSBaseline characteristics of patientsIn 2008, 345 patients were initially enrolled. A total of 332 patients completed the questionnaire, and 18 patients with missing data were excluded. In 2016, 304 patients were enrolled in the study. A total of 295 patients completed the questionnaire, and 18 with missing data were excluded. For both study periods, 591 patients were analyzed (Fig. 1). Comparing the two groups, the baseline characteristics were not significantly different in age (p=0.121), sex (p=0.075), and history of colonoscopy (p=0.941). However, significant differences were found in underlying disease (p=0.041), indications for colonoscopy (p<0.001), and educational level (p=0.041) (Table 1).
Patient sex preferences for colonoscopyIn 2008, 9.7% of male patients and 21.7% of female patients stated a preference with regard to the sex of their colonoscopist. Overall, 14.6% of patients stated a sex preference. In 2016, 20.3% of male patients and 29.9% of female patients had a sex preference, with an overall rate of sex preference of 24.9%. This was an increase compared with the overall sex preference of patients in 2008 (Fig. 2A). In 2008, 90% of male patients preferred a male colonoscopist, and the same preference was observed in 2016 (93.1%). However, 82.1% of female patients preferred a female colonoscopist in 2008, and this preference increased to 95% by 2016. This finding was statistically significant (odds ratio [OR], 2.678; 95% confidence interval [CI], 1.418т5.057; p=0.002).
Factors affecting sex preferenceIn multivariate analysis, patient sex OR, 4.404; 95% CI, 1.52т6.23; p=0.000), patient age (OR, 0.977; 95% CI, 0.961т0.992; p=0.004), and year of procedure (OR, 1.674; 95% CI, 1.028т2.752; p=0.038) were statistically significant factors in sex preference (Table 2). This shows that the increased sex preference in 2016 compared with that in 2008 was statistically significant (OR, 1.674; 95% CI, 1.028т2.752; p=0.038). In 2016, the probability that female patients will prefer female doctors was higher than in 2008 (OR, 2.678; 95% CI, 1.418т5.057; p=0.002).
The sex of the questioner, familial history of colon cancer, previous colonoscopy, underlying disease, residence, and history of sedation were not statistically related to patient sex preferences. In both 2008 and 2016, younger age influenced the sex preference of patients (Fig. 3A). No statistically significant difference was observed in sex preference according to educational background (Fig. 3B).
Reasons for and intensity of sex preferencesIn 2008, the reasons for sex preference in male patients were perception of doctor expertise (57%), embarrassment (29%), and gentleness (14%). In 2016, the reasons for sex preference in male patients were embarrassment (63%) and perceived doctor expertise (37%). In female patients, in both 2008 and 2016, the reasons for sex preference were stated as embarrassment, gentleness, and expertise (2008: 72%, 14%, 14%, 2016: 78%, 15%, 7%, respectively) (Fig. 4). During the last decade, the main reason for the preference by males for a male colonoscopist changed from perception of doctor expertise to embarrassment. When evaluating the intensity of sex preference, the proportion of patients who answered that they would wait for >30 min was 45.8% in 2008. In 2016, the proportion of patients who answered that they would wait for >30 min decreased to 31.8%, and the proportion of patients willing to wait for >1 h decreased to 13.0% (Fig. 5). When patients were asked if they would wait for a same-sex colonoscopist, fewer patients in 2016 than in 2008 answered affirmatively.
DISCUSSIONCommunication and understanding between physicians and patient are increasingly important [5]. In patient care, appropriate physicianтpatient relationships have a positive effect in promoting health. Sex is one of the most important factors to consider in a physicianтpatient relationship [10]. Recently, as the number of female physicians has increased worldwide, the opportunity to choose the sex of the physician is also increasing [2,5,6,8]. Patient embarrassment or shame during physical examination is a primary factor for increased same-sex preference [10]. Thus, several studies have been conducted about patient sex preferences in medical practice [11,12]. These studies have compared patient sex preference with regard to their physicians, with recent studies reporting that patients mainly preferred physicians of the same sex, particularly in Western countries [2,5,6].
Patient interest in the physicianтs sex may be high and may influence the patientтs attitude about undergoing colonoscopy. Few studies were conducted in the 2000s [2,3,7,8]. In a study of 150 patients conducted in the USA in 2002, 45% of female patients and 4.3% of male patients had a preference for a colonoscopist of the same sex [2]. In a UK study, the results were similar: 48% of female patients preferred a female colonoscopist, 3% of female patients preferred a male colonoscopist, 6% of male patients preferred a female colonoscopist, and 0% of male patients preferred a male colonoscopist [3].
In Korea, in 2005, 50.9% of male patients and 52.0% of female patients showed a sex preference [7]. However, in contrast to results of Western studies, among those who stated a sex preference, male patients preferred a male colonoscopist and half of the female patients preferred a male colonoscopist. In addition, in a 2008 Korean study of 358 women, one-third of the patients with a sex preference preferred a male colonoscopist (male patients: 13.4%, female patients: 32.1%). These results differed from those observed in Western countries, in which both male and female patients preferred a male colonoscopist. In Korea, particularly in the early 2000s, the physicianтpatient relationship was considered dependent and passive, and both male and female patients preferred a male colonoscopist [7]. In the early 2000s, there were few Korean female physicians. In addition, patients had a tendency to believe that male physicians had more authority, professionalism, and expertise [5,7,8]. However, the number of female colonoscopists is increasing. According to the Korean Society of Gastrointestinal Endoscopy, the number of newly certificated female endoscopic specialists in Korea was 114 (31.0%) in 2015, whereas this number was 38 (20.0%) in 2006. The number of female colonoscopists is approximately 1.5 times more today than 10 years previously. Within the last 10 years, the social activities of women have increased in Korean society, and the cultural perception of women has improved since the early 2000s. In addition, the overall cultural perception of women in Korea has become similar to that in Western countries because of the widening use of the Internet and media [13,14]. These broad cultural shifts are our reasons for assessing the changes in patient sex preferences with regard to the colonoscopist during the past decade.
In multivariate analysis, no difference was found based on the sex of the questioner. In 2008, Lee et al. [8] evaluated socioeconomic characteristics associated with the preference for a female colonoscopist among Korean women [5,8]. They showed that the preference for a female colonoscopist was related to younger patient age, employment status, educational level, and marital status [8]. In contrast, when multivariate analysis was used to calibrate the effects of other variables, only the patient sex and age were found to significantly influence their sex preference. We did not include marital and employment status in our study. However, in previous studies [5,8], younger female patient tendencies to be more educated, single, and employed were not corrected.
During the past decade, patient sex preference with regard to physicians has significantly increased [15]. In contrast to the early 2000s when female patients preferred a male colonoscopist, most female patients preferred a female colonoscopist in 2016. This trend is similar to that observed in previous Western studies, and is due to the above-mentioned shift in the social perception of women and the increased number of female doctors in Korea during the past decade. This is supported by the fact that the main reason for the preference for a male colonoscopist has changed from perception of physician expertise to embarrassment, as shown in Fig. 4. In Korea, sexual offenses have occasionally occurred during sedation. Considering that the sex of younger patients is related to their sex preference, we considered that privacy and anxiety about physical exposure are increasingly important for these patients.
Sex preference may vary among different regions and cultures. During the last decade, we showed that overall physician sex preference increased in Korea, and female patient preference for a female colonoscopist also increased. Through this study, we were able to show that providing patients with options concerning the sex of their colonoscopist can optimize patient comfort and satisfaction. This can improve patient compliance with screening colonoscopy and demonstrates consideration for the patient. In addition, consideration of physician conduct during a colonoscopy procedure is necessary because the main reason for sex preference is concern about body exposure. Therefore, studies on patient sex preference should be investigated in other medical specialties. Even within the same East Asian region, differences may be found, depending on the culture of each country. In Asia, ongoing research is needed on this issue.
This is the first study to demonstrate a change in patient sex preference over time, and comparing the difference with previous Korean studies is important. We identified changes in the reasons for and characteristics of sex preference, and found that colonoscopists should consider patient sex preference and concern about body exposure during endoscopy. Unlike previous studies, we used a method in which the physician directly spoke with the patient. In addition, we used multivariate analyses of several variables that could affect sex preference. However, there was a limitation in that the sex preference was lower than that reported in previous studies. This could be attributed to the questioner speaking directly with the patient.
In conclusion, our study showed that patient sex preference with regard to their colonoscopist has overall increased in Korea, and an increase in female patient preference for a female colonoscopist was observed during the study period. This study suggests that the sex of the colonoscopist can affect overall patient satisfaction, as well as the access to and compliance with colonoscopy. Based on these results, consideration of patient sex preference for a physician and patient embarrassment would be helpful in achieving desirable outcomes in endoscopic procedures.
AcknowledgmentsThis research was supported by a 2014 Weolbong grant from the Korean Gastrointestinal Endoscopy Research Foundation and by a grant from Korea University.
Fig.Т 3.(A) Relationship between age and sex preference. (B) Relationship between educational level and sex preference. 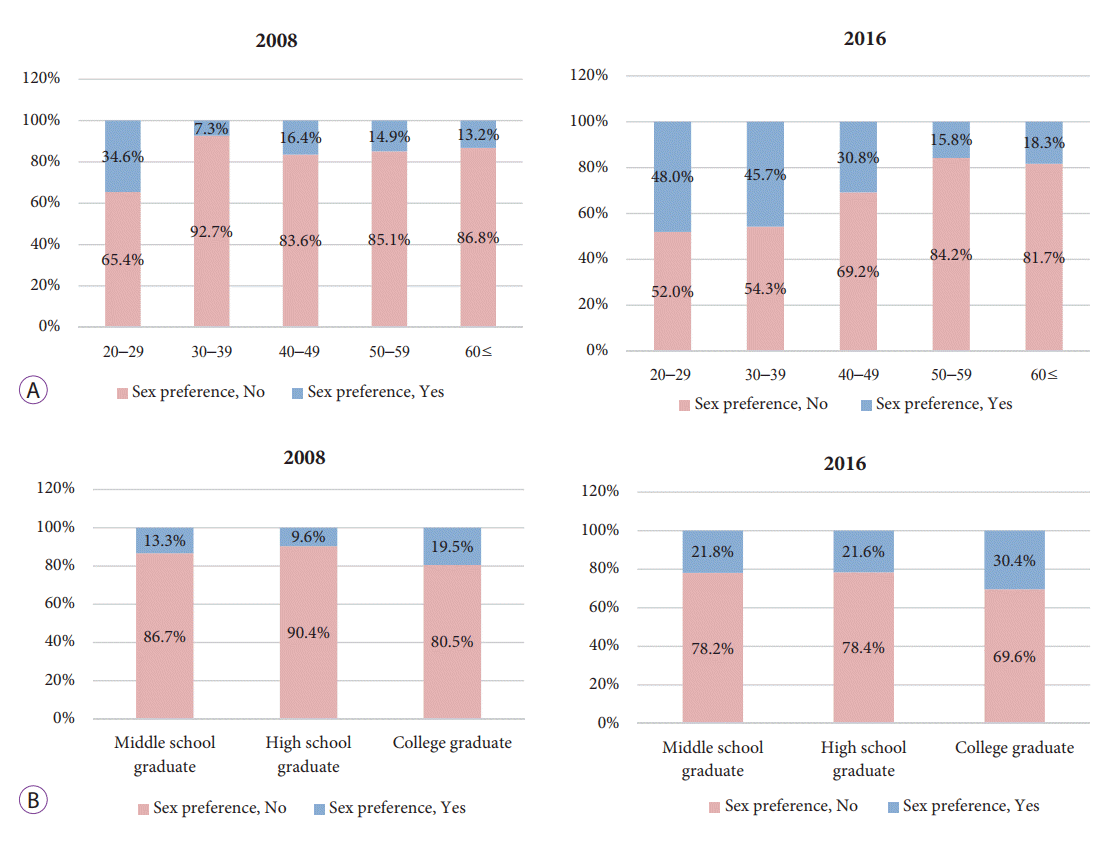
Fig.Т 5.Intensity of sex preference: if the patient stated a preference for the sex of their colonoscopist, how much time would they wait for colonoscopy? 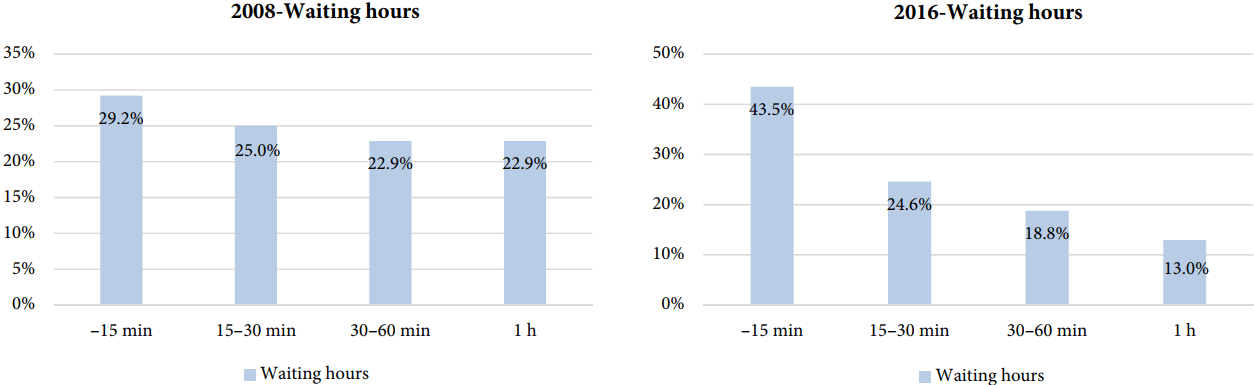
TableТ 1.Baseline Characteristics
TableТ 2.Logistic Regression Analysis of Gender Preference
REFERENCES1. Winawer SJ, Zauber AG, Ho MN, et al. The national polyp study. Eur J Cancer Prev 1993;2 Suppl 2:83т87.
2. Varadarajulu S, Petruff C, Ramsey WH. Patient preferences for gender of endoscopists. Gastrointest Endosc 2002;56:170т173.
3. Fidler H, Hartnett A, Cheng Man K, Derbyshire I, Sheil M. Sex and familiarity of colonoscopists: patient preferences. Endoscopy 2000;32:481т482.
4. Menees SB, Inadomi JM, Korsnes S, Elta GH. Women patientsт preference for women physicians is a barrier to colon cancer screening. Gastrointest Endosc 2005;62:219т223.
6. Shah DK, Karasek V, Gerkin RD, Ramirez FC, Young MA. Sex preferences for colonoscopists and GI physicians among patients and health care professionals. Gastrointest Endosc 2011;74:122т127.e2.
7. Kim JH, Lee JH, Park EH, et al. Patientsт gender preference for colonoscopist. Korean J Gastrointest Endosc 2005;31:25т31.
8. Lee SY, Yu SK, Kim JH, et al. Link between a preference for women colonoscopists and social status in Korean women. Gastrointest Endosc 2008;67:273т277.
9. Govender V, Penn-Kekana L. Gender biases and discrimination: a review of health care interpersonal interactions Glob Public Health. 2008;3(Suppl 1):90т103.
10. Kerssens JJ, Bensing JM, Andela MG. Patient preference for genders of health professionals. Soc Sci Med 1997;44:1531т1540.
11. Reid I. Patientsт preference for male or female breast surgeons: questionnaire study. BMJ 1998;317:1051.
12. Haar E, Halitsky V, Stricker G. Factors related to the preference for a female gynecologist. Med Care 1975;13:782т790.
13. Farraye FA, Wong M, Hurwitz S, et al. Barriers to endoscopic colorectal cancer screening: are women different from men? Am J Gastroenterol 2004;99:341т349.
14. Maynes K. Korean perceptions of chastity, gender roles, and libido; from kisaengs to the twenty first century. Grand Valley Journal of History 2012;1:Article 2.
|
|
|||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
