CME for
KSGE members
Kim and Lee: A rapidly growing round mass in the gallbladder
Quiz
A 72-year-old man was admitted for an abnormal gallbladder lesion on follow-up abdominal computed tomography (CT). He had a surgical history of hemicolectomy for sigmoid colon cancer two years ago. A physical examination of the abdomen showed a flat and non-tender abdomen. Blood chemistry and tumor marker tests, including CA19-9 results, were all within normal ranges.
Abdominal CT during the follow-up period after surgery showed minimal ovoid-shaped gallbladder wall thickening in the fundus lesion, suggesting fundal adenomyomatosis ( Fig. 1A). Therefore, a follow-up CT was performed six months later for gallbladder lesions, which revealed an increased cystic mass lesion on the fundus of the gallbladder ( Fig. 1B). Endoscopic ultrasonography (EUS) later revealed an approximately 2├Ś1 cm elliptical wall thickening on the fundus ( Fig. 2). The mucosal and serosal layers were well-preserved, and multiple internal hyperechogenic spots and hypoechoic lesions were mixed within a round, mass-like lesion. Moreover, no bile duct dilatation or lymph node enlargement was observed around the bile duct. What is the most likely diagnosis?
Answer 
The patient underwent laparoscopic cholecystectomy because of a rapidly growing mass-like lesion, which made it difficult to rule out malignancy. Abdominal CT and EUS cannot differentiate between adenomyomatosis and adenoma. In addition, the role of magnetic resonance imaging (MRI) is limited in making a definite diagnosis compared with CT and EUS. Therefore, we decided to perform surgery instead of further follow-up or evaluation, such as an MRI. Histopathological examination of the resected gallbladder showed a Rokitansky-Aschoff sinus in the lower power field (├Ś10, Fig. 3A) and foamy histiocytes, lymphocytes, and multinucleated giant cells (├Ś100, Fig. 3B), suggesting xanthogranulomatous cholecystitis. In the present case, a rapidly growing mass in the gallbladder was finally diagnosed as xanthogranulomatous cholecystitis, which is a rare benign inflammatory disease of the gallbladder. However, it may be misdiagnosed as carcinoma of the gallbladder on imaging. 1-3 Usually, imaging features of xanthogranulomatous cholecystitis and carcinoma of the gallbladder are similar and difficult to differentiate, and sometimes both conditions can co-exist. Therefore, cholecystectomy is the only definitive treatment for suspected xanthogranulomatous cholecystitis. Xanthogranulomatous cholecystitis is characterized by a focal or diffuse destructive inflammatory process, with the accumulation of lipid-laden macrophages, fibrous tissue, and acute and chronic inflammatory cells microscopically. 1 The pathogenesis of xanthogranulomatous cholecystitis may be related to extravasation of bile into the gallbladder wall from rupture of Rokitansky-Aschoff sinuses or by mucosal ulceration. This event induces an inflammatory reaction in the interstitial tissue, whereby fibroblasts and macrophages phagocytose the biliary lipids in bile, such as cholesterol and phospholipids, leading to the formation of xanthoma cells. 1,4,5 Lipid-laden macrophages are of two morphological types: rounded foamy macrophages and spindle-shaped cells with more granular cytoplasm and elongated nuclei. Other findings include the presence of cholesterol clefts, lipid droplets, hemosiderin deposits, and extravasated bile. 1 These pathologic characteristics may result in mixed hyperechoic and hypoechoic echotextures on EUS. 6
In this case, focal small wall thickening of the gallbladder was initially suspected as fundal-type adenomyomatosis. However, a CT scan performed for colon cancer surveillance and follow-up imaging revealed a rapidly growing mass. Despite EUS findings, cholecystectomy was performed because it was difficult to exclude malignancy. Finally, the rapidly growing gallbladder fundus lesion was diagnosed as xanthogranulomatous cholecystitis.
Fig.┬Ā1.
Abdomen computed tomography (CT) findings. (A) Enhanced CT showed focal enhancement and wall thickening on the fundus (yellow arrow) of the gallbladder without disruption of the wall layer. (B) A follow-up CT showed similar findings, but with enlarged enhancing wall thickening and a hypodense lesion on the gallbladder fundus (yellow arrow). Direct liver invasion or wall disruption of the gallbladder was not definitive. 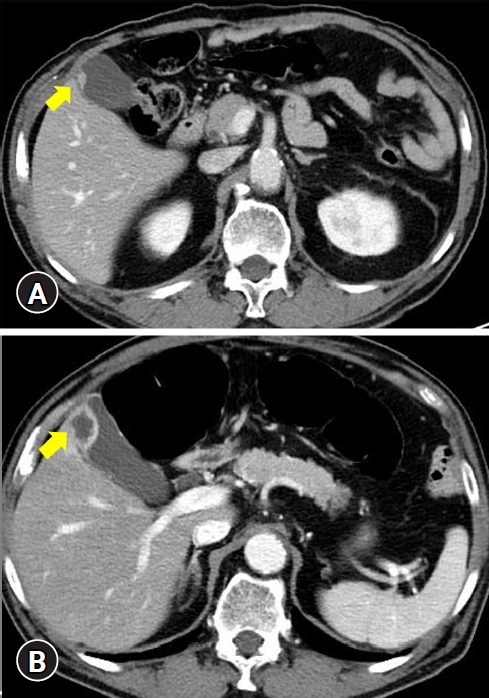
Fig.┬Ā2.
Endoscopic ultrasound image shows about 2├Ś1 cm sized elliptical wall thickening without disruption of the wall layer. Internal echogenicity was mixed with diffuse hyperechoic spots and hypoechoic lesions. 
Fig.┬Ā3.
Pathologic features of the resected specimen. (A) A Low-power field (hematoxylin and eosin stain, ├Ś10) showed Rokitansky-Aschoff sinuses resulting from hyperplasia and herniation of epithelial cells through the fibromuscular layer of the gallbladder wall. (B) A high-power field (hematoxylin and eosin stain, ├Ś100) revealed abundant infiltration of foamy histiocytes, lymphocytes, and multinucleated giant cells. 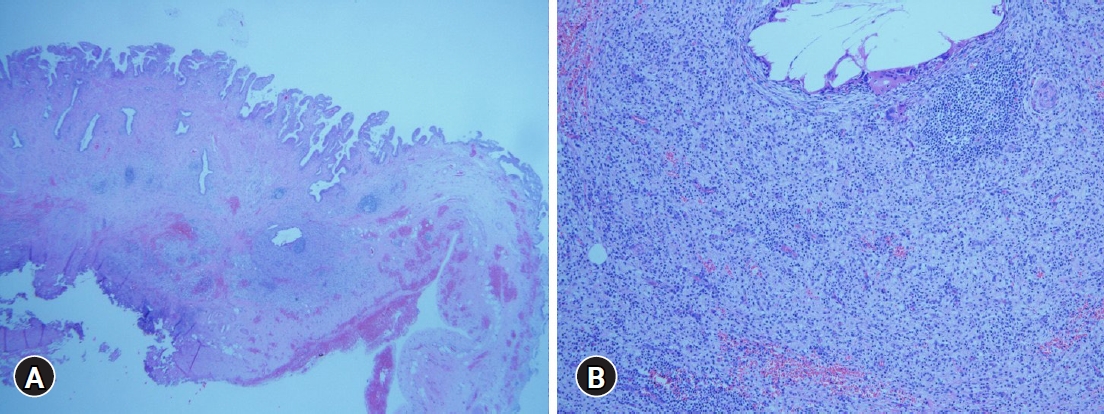
|
|












