INTRODUCTION
Gastric mesenchymal tumors (GMTs) are accidentally discovered as protruding firm subepithelial lesions during upper endoscopy, particularly in national gastric cancer screening programs in Korea [1]. These tumors usually appear as spindle-shaped cells and display smooth muscle or nerve sheath differentiation on histopathology. Most GMTs are gastrointestinal stromal tumors (GISTs) derived from interstitial cells of Cajal [1,2]. Because GISTs have a risk of metastasis, particularly to the liver and peritoneum, even after surgery for localized diseases [3,4], all GISTs are considered potentially malignant and candidates for resection, especially when they are larger than 1 cm [4-6].
Differentiating GISTs from benign mesenchymal tumors, such as schwannomas or leiomyomas, is important to ensuring proper clinical decisions. Endoscopic ultrasonography (EUS) is the most useful diagnostic modality for evaluating gastrointestinal subepithelial lesions because it enables the demonstration of margins, echogenicity, layer of origin, and detailed morphology [7-9]. Although many studies have attempted to differentiate GISTs from benign GMTs using EUS, the results are controversial [9,10]. Because of subjective interpretation of EUS image findings, limitations such as poor interobserver agreement persist in the analysis of the characteristic features of GMTs [11,12]. To overcome these limitations, digital image analysis is expected to help endoscopists improve GMT diagnosis accuracy. Here we summarize the usefulness and future of digital EUS image analysis for GMTs based on published reports and our experience.
ENDOSCOPIC ULTRASONOGRAPHY FEATURES OF GASTRIC MESENCHYMAL TUMORS
During EUS examinations of GMTs, endoscopists should carefully recognize the following features: (1) tumor location; (2) presence of mucosal ulceration on endoscopy and/or EUS; (3) maximal diameter; (4) echogenicity relative to the surrounding normal proper muscle layer (hyperechoic, isoechoic, or hypoechoic); (5) homogeneity (homogenous or heterogeneous); (6) presence of cystic spaces, hyperechogenic spots, and calcification; (7) presence of a marginal halo and lobulation; (8) regularity of the marginal border (regular or irregular); and (9) tumor growth pattern (inside or outside the gastric wall) [13]. Of them, several EUS features of GMTs can provide important clues to ensure the correct diagnosis and appropriate management (Fig. 1). According to our previous studies, tumor location, tumor echogenicity relative to the surrounding normal proper muscle layer, homogeneity, and presence/absence of hyperechogenic spots and marginal halo are helpful for diagnosing GMTs (Table 1).
Leiomyoma
Leiomyomas are benign tumors that originate from the muscularis mucosa or the muscularis propria of the gastrointestinal tract. Gastric leiomyomas are usually found in the cardia and upper body. On EUS, leiomyomas are well-circumscribed homogeneously hypoechoic lesions with an echogenicity that is similar to that of the surrounding proper muscle layer. Calcifications are relatively common in leiomyomas (6.5%ŌĆō18%) but rare in GISTs and schwannomas (0%ŌĆō3.5% and 0%ŌĆō3.7%, respectively) [14-16].
Schwannoma
Schwannomas are tumors of spindle cells that arise from the benign nerve sheath of Schwann cells. Gastric schwannomas are usually found at a rate of 57%ŌĆō81% in the body, 7%ŌĆō40% in the antrum, and 0%ŌĆō29% in the fundus, especially in middle-aged women [16-18]. On EUS, they are heterogeneously or homogeneously hypoechoic lesions with decreased echogenicity relative to the surrounding proper muscle layer [16]. Since schwannomas have a peripheral lymphoid cuff around the lesion, a prominent marginal halo is seen on EUS at a rate of 71%ŌĆō89% [16-18]. However, the marginal halo is not a unique EUS finding of schwannomas; rather, it is also frequently observed in GISTs but with a different mechanism. GISTs represent a capsule-like structure that is partially or completely circumscribed by the surrounding proper muscle. Therefore, the marginal halo of GISTs is thinner than that of schwannoma [9,10].
Gastrointestinal stromal tumors
GISTs are the most commonly discovered GMTs and have malignant potential. Gastric GISTs are usually found in the body and fundus (in 46%ŌĆō58% and 21%ŌĆō33%, respectively) but rarely found in the antrum and cardia (13%ŌĆō18% and 2%ŌĆō8%, respectively) [14,19]. Many previous studies attempted to demonstrate the ability of EUS to differentiate GISTs from other GMTs, but the results are inconsistent. On EUS, GISTs show hypoechoic and heterogeneous echo patterns with a marginal halo and hyperechoic spots. The echogenicity of GISTs is slightly higher than that of the surrounding proper muscle layer [9]. Several EUS features such as size, irregular margin, cystic change, presence of hyperechogenic foci, and peritumoral lymphadenopathy are suggested as factors predictive of a high risk of malignant potential; [8,20] according to our previous study, only tumor size (>3.5 cm) is the most accurate factor for predicting malignancy [9].
DIGITAL ENDOSCOPIC ULTRASONOGRAPHY IMAGE ANALYSIS FOR GASTRIC MESENCHYMAL TUMORS
We have previously reported that hyperechogenic spots, a peripheral halo, heterogeneity, and hyperechogenicity in comparison with the surrounding proper muscle layer are important for differentiating GISTs from other GMTs [9]. There is high sensitivity (89.1%) and specificity (85.7%) in the presence of at least two of these four features for predicting GISTs. However, as abovementioned, the interpretation of EUS images is subjective, which can result in poor interobserver agreement. To overcome this limitation, we must objectively analyze the EUS images of GMTs.
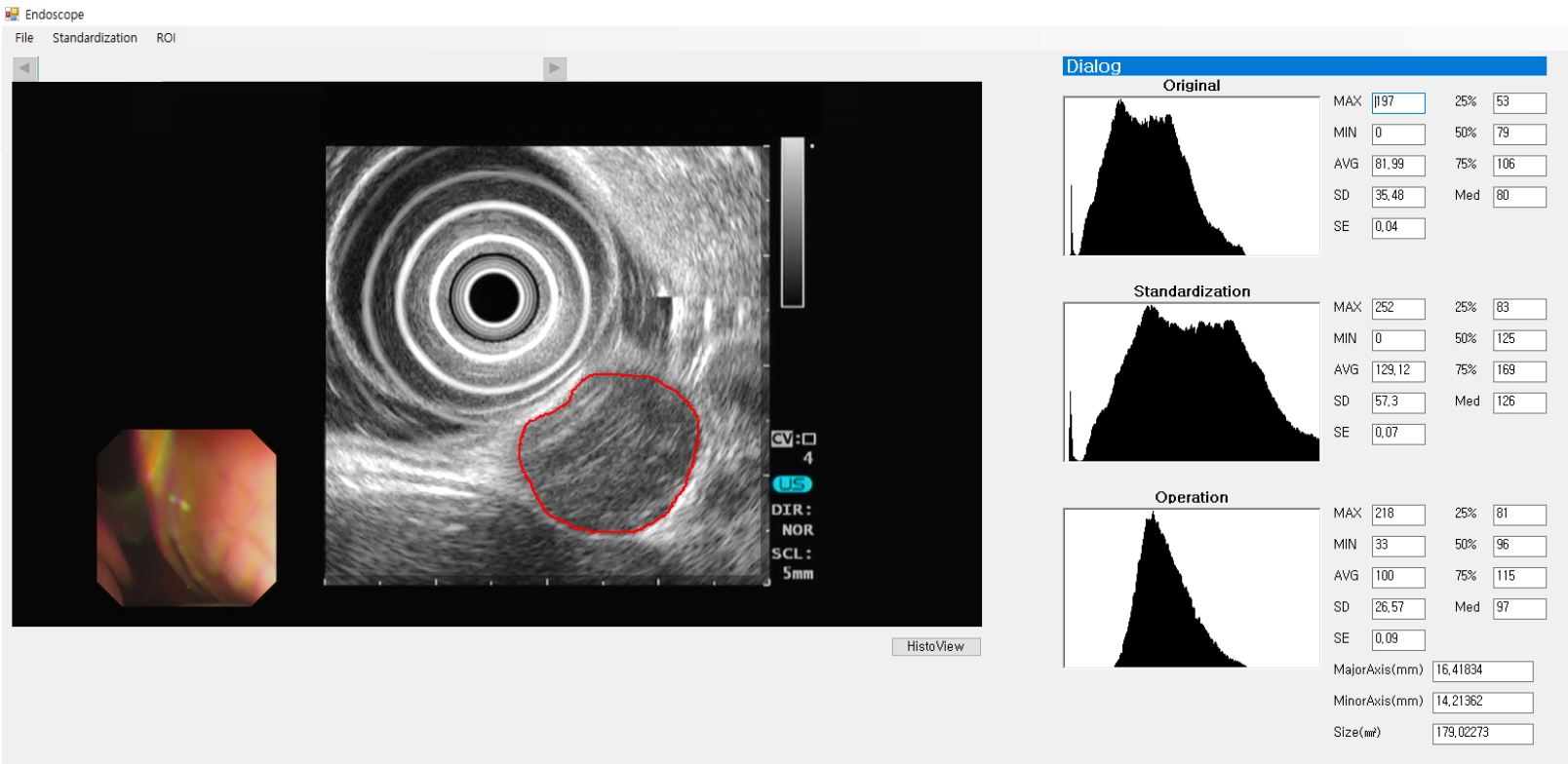
However, EUS images display different characteristics according to actual EUS settings such as gain and contrast, different echoendoscopes (mechanical vs. electronic), and EUS systems used during EUS examinations. Thus, the standardization of EUS images is required to minimize these differences. Accordingly, in our previous studies, we selected the least variable portion of the EUS images such as the outer hyperechoic rim and anechoic center of the echoendoscope and processed the standardization [21,22]. Next, we attempted to find a method to objectively evaluate EUS findings such as homogeneity and echogenicity grades. EUS images are pixels that compose black and white images, and the brightness value (range, 0ŌĆō255) represents their echo density. Therefore, we thought that analysis of the brightness values can be an appropriate method to evaluate echogenicity level and heterogeneity degree. As a result, the echogenicity level and heterogeneity degree were expressed as mean (Tmean) and standard deviation (TSD) of the brightness values. Based on the above processes, we developed a diagnostic system using the digital EUS image analysis of GMTs (Fig. 2).
In our first study of 65 GMTs, the Tmean and TSD were significantly higher in GISTs than in leiomyomas and schwannomas [22]. When a receiver operating characteristic (ROC) curve was created to identify the best sensitivity and specificity cutoff values of Tmean and TSD for differentiating GISTs from leiomyomas or schwannomas, the sensitivity and specificity was almost optimized when Tmean was Ōēź65 and TSD was Ōēź75 for predicting GISTs. There was high sensitivity (94%) and specificity (80%) in the presence of at least one of these two findings for predicting GISTs.
Next, we focused on GMTs measuring 2ŌĆō5 cm. According to recent guidelines for gastric subepithelial tumors, when GMTs are smaller than 2 cm, they can usually be followed by periodic endoscopy or EUS once or twice a year until the tumors increase in size or become symptomatic, even if they are diagnosed as GISTs later [13,21]. However, surgical resection is recommended for GMTs measuring >5 cm. If a GMT measures 2ŌĆō5 cm, the clinical decision process can be shared with patients regarding whether to perform a histopathological diagnosis examination (for example, by EUS-guided fine-needle aspiration/biopsy or by deep biopsy via endoscopic submucosal dissection) or whether the patient requires surgical resection. Therefore, we tried to develop a scoring system to predict GISTs in 103 GMTs measuring 2ŌĆō5 cm using digital EUS image analysis [21]. Similar to our previous study, Tmean and TSD were significantly higher in GISTs than in non-GIST tumors. In addition, patients with GISTs were older than those with nonGIST tumors. When ROC curves were created, the sensitivity and specificity were almost optimized for differentiating GISTs from non-GIST tumors when the critical values of age, Tmean, and TSD were 57.5 years, 67.0, and 25.6, respectively. Based on the ╬▓-coefficient values of multivariate analysis, we created a GIST predicting scoring by assigning 3 points for Tmean Ōēź67, 2 points for age Ōēź58 years, and 1 point for TSD Ōēź26 (Table 2).
GMTs with 3 or more points predicted GISTs with a sensitivity of 86.5% (95% confidence interval [CI], 80.3%ŌĆō91.0%), specificity of 75.9% (95% CI, 60.0%ŌĆō87.4%), and accuracy of 83.5% (95% CI, 74.6%ŌĆō90.0%). Considering the diagnostic yield of EUS-guided fine-needle aspiration/biopsy for subepithelial tumors is 60%ŌĆō85% [23-25], the GIST predicting scoring system can to be useful for ensuring appropriate clinical decision. In another study using an artificial neural network based on the multilayer perceptron architecture on EUS images of gastric subepithelial tumors, the authors showed high accuracy for the differential diagnosis of malignant subepithelial tumors (GISTs and carcinoid tumors) from lipomas [26]. The model was reported as ŌĆ£goodŌĆØ for the differentiation of carcinoid tumors and GISTs and ŌĆ£excellentŌĆØ for the differentiation of lipomas, with areas under the ROC curve of 0.86, 0.89, and 0.92, respectively.
Studies published to date on digital EUS image analysis for GMTs are summarized in Table 3. However, these studies are subjected to several limitations. First, all three studies are based on single-center experiences. As aforementioned, EUS images vary according to different clinical settings such as contrast, gain, and differences in EUS systems and echoendoscopes. Even standardization process cannot overcome these differences completely. Therefore, the results of previous studies require validation in various clinical settings. Second, because all published studies were retrospective, bias in the EUS image review process might have been unavoidable. In our studies, we selected the EUS images with the highest quality to perform the digital image analysis. However, during EUS examination, at least 10 EUS images were usually taken to determine the characteristics of GMTs; this would help compensate for the limitations of retrospective research. Accordingly, we plan to conduct a large-scale, multi-center prospective study to validate the digital EUS image analysis system used to predict the histopathology of GMTs.
CONCLUSIONS
EUS provides useful information for the differential diagnosis of GMTs. Furthermore, digital EUS image analysis can provide additional help to endoscopists by decreasing interobserver variability and increasing diagnostic accuracy by enabling the objective analysis of EUS images. Future digital EUS image analysis systems will be embedded in the EUS system to enable real-time analysis. It is true that this system helps endoscopists make clinical decisions and make the differential diagnosis in patients with GMTs. However, before being used in real practice, these technological advances will require validation in prospective multicenter studies.